CHARLESTON, W.Va. — Kristi Haynes knew she had a problem when her eyes turned the color of traffic paint. Haynes had been feeling strangely tired, but she didn’t have many opportunities to look at herself in a mirror because she’d been homeless for a few months. Her fiance noticed her yellow eyes and freaked out. And that’s how Haynes knew she had caught the disease so many of her friends already had: hepatitis A.
Hepatitis A, a vaccine-preventable disease that attacks the liver and is spread by contaminated fecal matter, is a scourge in developing nations with poor sanitation systems. Imported contaminated food is typically to blame when the disease occurs in developed countries.
But U.S. cases of the disease have tripled in 2018, and the outbreak has nothing to do with imported food.
Hepatitis A is spreading among drug-using and homeless populations, with explosions of the disease moving from California to states such as Kentucky, West Virginia, Ohio, Indiana and Missouri.
The toll has been vast: At least 10,582 people have been reported infected so far this year alone, a large number of whom have required extensive — and thus expensive — hospitalizations. Hepatitis A inflicts what feels like severe flu symptoms: nausea, fever, dizziness, overall lethargy, and jaundice. Without treatment, severe cases of hepatitis A can cause liver failure. At least 80 people have died from this outbreak.
States, counties, and cities have spent millions to fight their local outbreaks, but the money doesn’t address the root causes of the problem: a decaying public health infrastructure, devastated by years of funding cuts, that can’t fully meet the needs of a population driven to homelessness and devastated by the opioid epidemic.
“Unfortunately, I see this hepatitis A outbreak as a symptom of the fraying social safety net,” said Dr. Jeff Duchin, a public health officer for Seattle and King County, Washington.

‘A New Normal’
Prior to 1995, when hepatitis An antibody was first authorized in the U.S., around 21,000 Americans were determined to have hepatitis An every year, as per the Centers for Disease Control and Prevention. In 2006, the CDC prescribed all youngsters be immunized, and numerous states presently necessitate that kids get the antibody before going to class.
The arrival of the antibody and the spread of vaccination caused the number of new instances of the infection to dive. For the initial two decades after the landing of the immunization, most episodes of hepatitis An in the U.S. were associated with imported defiled nourishment sources — like the 2016 episode because of solidified strawberries or the 2013 flare-up from pomegranate seeds. On a lot littler scale, the U.S. has likewise recently observed floods in cases among gay, androgynous and other men who have intercourse with men.
So when San Diego County in California saw a spike in hepatitis A cases beginning in late 2016 and there didn’t seem, by all accounts, to be a hidden sustenance source, the area was gotten unsuspecting. The area wellbeing division found the malady was spreading through unsanitary living conditions in makeshift camps and among medication clients who were too old to even think about having been inoculated before going to class. Amid the pinnacle of the flare-up that falls, the area showered its boulevards with blanch. The wellbeing office propelled a huge immunization battle, included hand-washing stations and new washrooms, and gave out human crap packs that individuals could use to discard their waste on the off chance that they didn’t have normal access to a restroom.
When San Diego subdued the flare-up toward the beginning of 2018, about 600 individuals had been contaminated and 20 had kicked the bucket. It was only the start.
The San Diego strain of hepatitis A started to spring up across the country toward the finish of 2017 and the start of 2018, in Utah and afterward in Kentucky, Indiana and West Virginia. Michigan saw a blast of an alternate strain of the infection.
Indiana before long made the extreme stride of issuing a tourism warning, recommending that its occupants get immunized this spring before making a beeline for Louisville for the Kentucky Derby in view of the developing flare-up there.
“Sickness doesn’t perceive outskirts when there are flare-ups in neighboring states,” said Pam Pontones, Indiana’s agent state wellbeing magistrate and state disease transmission specialist.
As it kept on moving east, the ailment spread principally through the medication utilizing populace. Unsanitary and at times transient conditions related with medication use put that populace in danger for presentation to the debased fecal issue, wellbeing offices state. There is additionally some proof to propose a conceivable association between the sickness and intravenous medication use, as indicated by Dr. Sapna Bamrah Morris, who helps lead the CDC’s reaction to hepatitis A.
“These are every one of the side effects of the expense and human toll the narcotic plague is taking,” Rahul Gupta, who was the leader of the West Virginia Department of Health and Human Resources until November, told HuffPost in September. “It’s considerably more an indication of the occasions we’re in and the huge scourge, the torrent of transferable infection that can occur.”
What made these episodes hard to stop, general wellbeing authorities state, is that they were harming the general population who are hardest to achieve: the individuals who are destitute, transient or utilizing medications, and who don’t believe the medicinal services framework following quite a while of disparagement.
If these large hepatitis A outbreaks were happening, for example, on college campuses, you’d probably see a different level of energy around getting resources mobilized to respond to them more comprehensively.
Public health departments had to partner with homeless shelters, soup kitchens and needle exchanges to find these cases of hepatitis A. They set up vaccine drives, deployed strike forces of nurses and staff across cities, sent out mobile vaccine units to far away rural areas. That all takes time and money and effort — and the disease is still spreading.
“Reaching the at-risk populations that are currently affected is extremely resource intensive and everyone has limitations on the resources they have,” said Morris from the CDC.
Health departments also have “competing priorities,” she said, like the onslaught of the flu season.
Duchin put it a bit more bluntly.
“If this large hepatitis A outbreaks were happening, for example, on college campuses, you’d probably see a different level of energy around getting resources mobilized to respond to them more comprehensively,” he said.
The entire outbreak demonstrates how public health is failing people most in need of protection, said Jeffrey Howard, the commissioner of Kentucky’s public health department. When the CDC finally issued an advisory to health departments nationwide in June, cases were nearing 2,000 for the year. Now there are closing in on 11,000.
“It is always clear that inequities and disparities in health and health outcomes exist — and they exist across this country,” Howard said. “We have to do a better job of protecting that vulnerable population and I think that’s the responsibility of all of public health.”

Yet all the while, hepatitis A has continued to spread despite health departments’ efforts. And the problem gets worse as those outbreaks move from urban centers to more rural areas that have less public health infrastructure, Howard said. Kentucky and West Virginia have seen such a pattern and have the worst outbreaks to date with 3,265 cases and 2,137 cases, respectively. They’re still seeing new cases every week.
“My guess is we’re going to see a new status quo with hepatitis A,” Howard said. “Hepatitis A is not going to be a rare disease as it used to be in this country. It’s probably going to be a new normal.”
Decaying Infrastructure
Officials point to declining public health funding to explain the explosion of this preventable disease. More than 56,000 local health department jobs were lost nationwide between 2008 and 2017, according to the National Association of County and City Health Officials (NACCHO). In that time, STD rates have skyrocketed, the opioid crisis now claims more than 115 lives a day, and 80,000 people died of the flu last year.
“As funding cuts happen all along over years, it’s really the public health infrastructure that erodes,” said Lilly Kan, the senior director for infectious disease and informatics at NACCHO. “It continues to be a smoldering issue, but then when you have fires like outbreaks like hepatitis A, then it becomes obvious.”
Nowhere were the consequences of public health cuts more evident than in West Virginia, where Haynes contracted hepatitis A. The state instituted a 24 percent cut in state aid to public health departments in 2016, and several leadership positions remained unfilled as the outbreak spread across the state.
“We’ve been able to manage, and counties that don’t have our resources cannot,” said Dr. Michael Kilkenny, the physician director at the Cabell-Huntington Health Department. “The state is overtaxed and is relying on the CDC.” But the CDC, which has competing priorities and a limited budget, can only do so much.
Kilkenny told WV Public Radio in 2016 that funding cuts “would really cripple” surveillance efforts for all sorts of diseases.
“If we stop watching for those diseases, those diseases will spread, people will get sick and some of those people will die,” he said at the time.

West Virginia’s hepatitis An episode is currently the second-most exceedingly bad in the nation. Twelve of them in excess of 2,000 West Virginians who have been determined to have the ailment this year have kicked the bucket.
Wellbeing offices over the state have lost key staff; the state as of now has a break chief of general wellbeing. The staffing issues are especially critical in Kanawha County-Charleston ― the core of the episode, with 782 cases to date. The head of clinical administrations at the Kanawha-Charleston Health Department left for the current year, as did the head of an organization and the head of wellbeing advancement and wellbeing, as per the previous leader of the office. Five clerical specialists were given up because of spending cuts in 2017.
Dr. Michael Brumage, the previous office head, withdrew for the current year in the midst of open reaction over a disputable needle trade in Charleston that close down in February. What’s more, Brenda Isaac, the leader of the region’s wellbeing board, surrendered in October, saying she had turned into a “lightning bar” in the mayoral race, which was to a great extent a choice on the needle trade. The break leader of the city’s general wellbeing division is working low maintenance.
“It was an extremely appalling situation that exhausted the wellbeing branch of assets right when they required it most,” said Brumage, who is presently the aide dignitary for general wellbeing practice and administration at the West Virginia University School of Public Health. “Indeed, even under the best of conditions, it’s hard to enroll staff as financing has been sliced throughout the years.”

The Kanawha-Charleston Health Department didn’t move fast enough to combat hepatitis because it was distracted by the fight over the needle exchange, said Dr. Angie Settle, the CEO and executive director of West Virginia Health Right, a free health care clinic in Charleston. The county didn’t ramp up its efforts until new cases were peaking in the summer, added Ellen Allen, the executive director of Covenant House, a day shelter in downtown Charleston. Both organizations have played important roles in fighting the outbreak.
“We requested the health department to come in February, but we felt like we kept it too limited in scope,” Allen said. “We should have gotten our arms around this in the spring.”
Human Poop Bags
The primary populations affected by the outbreak — homeless people and drug users — are served by Covenant House, which has seen a sharp uptick in people coming through the door as the West Virginia economy has struggled in recent years.
Briana Martin, who manages the needs of people who drop in each day at Covenant House, knows at least 10 people in the day shelter who have been infected. She makes sure to wash her hands after interacting with people who have been exposed to hepatitis A. For those who haven’t been vaccinated against the disease, all it would take to contract hepatitis A would be to shake hands with someone who has it or touch the bathroom door before eating.
The health department has been handing out bags filled with wipes, a toothbrush, toothpaste, two water bottles, toilet paper, hand sanitizer, gloves, detailed sanitary instructions — and a poop bag. Over 85 people at Covenant House had received the kits as of September.

In any case, clean issues endure. Allen said her staff regularly tidies up crap outside the asylum. She has asked for increasingly outside restrooms, yet nothing has changed — and the asylum is just open 8 a.m. to 4 p.m.
It’s simply one more sign that things keep on exacerbating for those without a security net, as indicated by Allen.
“I’ve never observed anything like this,” she said. “I’ve been in charitable labor for a long time now and simply the most recent year the quickening and the decline in the prosperity of individuals — it’s lamentable.”
All of the 20 or so individuals at Covenant House one evening this September said they had known about hepatitis A. Yellow signs with intense letters encouraging individuals to get inoculated spotted the dividers.
Haynes, who asked not to be captured, was there doing her clothing. A moderately aged man who was visiting the safe house and did not have any desire to be recognized said he had a companion who had passed on in the wake of contracting hepatitis A, which confused his basic hepatitis B and C.
Terrell, a Covenant Houseguest who declined to give his last name, sat outside the entryways for a couple of hours before advancing into prod the staff. Yet, when gotten some information about hepatitis A, he addressed rapidly. “I’ve seen individuals going to kick its bucket — hold up till they’re going to pass on before they go in,” he said. “Is it safe to say that it isn’t a third-world malady and some crap?”

The Damage Done
The monetary expenses of these flare-ups have been high, regardless they’re rising.
San Diego County gauges it burned through $12.5 million to subdue its episode, which is one-quarter the span of West Virginia’s. Kentucky has apportioned $2 million so far to the immunization alone, which doesn’t tally government cash. The fundamental hospitalization costs are galactic, which Brumage said winds up influencing the two clinics and citizens on the grounds that such a significant number of individuals from the in danger populaces are uninsured.
“Those are extremely broad hospitalizations that itself would be a few million,” said Gupta, West Virginia’s previous general wellbeing magistrate.
This doesn’t start to represent alternate assets, for example, time, that general wellbeing divisions and network organizations have put toward engaging the flare-ups.

And news of an outbreak can devastate a local economy.
Popular fast food restaurants in West Virginia have taken a massive hit, said Tri-State Restaurant Association spokesman Mike Kirtner. The organization was formed after Ohio, Kentucky and West Virginia saw hepatitis A cases take off. Hepatitis A cases have shut down several restaurants in the Charleston area this year, and Kirtner said one major chain lost 70 percent of its business in a single day after a case of hepatitis A was reported. Waitresses at affected restaurants have seen their tips decrease, Kirtner said, sometimes from as much as $300 a day to just $50.
Blame Game
Legislators, nearby TV news and general society have faulted pretty much everything aside from the absence of general wellbeing financing for the flare-up in West Virginia.
“Everything originated from eateries,” Danny Jones, Charleston’s active city hall leader, told HuffPost.
Be that as it may, none of the West Virginia cases have been followed to nourishment sullying. In any case, Kirtner stated, eatery specialists, who are at a lot higher hazard for the malady, are excessively spoken to among intravenous medication clients.
Jones additionally censured the wellbeing office for the flare-up, saying it “got it somewhat late.” But the genuine issue, he contended, was a “needle process” that pulled in bothersome individuals to Charleston.
“Too many free dinners attracting individuals,” he said.
Talk that way — the possibility that administrations helping the destitute and medication utilizing individuals are devastating Charleston — is winding up more standard.
A private Facebook aggregate called “Charleston Has Had Enough” faults “addicts, bums, cheats, unsafe individuals, most from out of state,” for the region’s developing issues and urges clients to “post your photographs of troublemakers.”
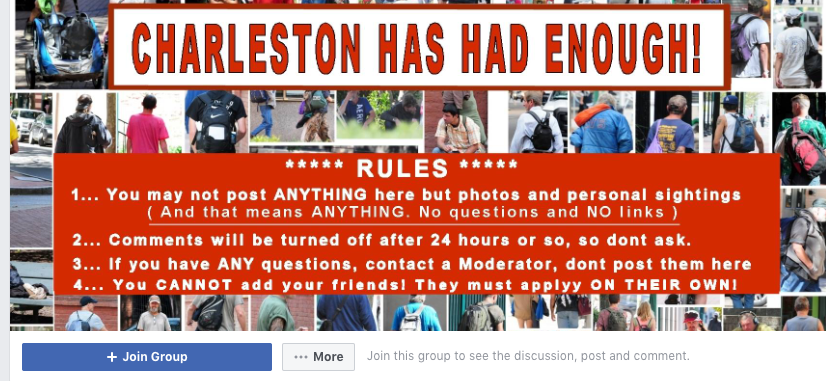
The gathering has in excess of 4,600 individuals, which is practically identical to around 10 percent of the city’s populace. Clients post unflattering photographs of individuals who seem, by all accounts, to be among the region’s destitute and medication clients, and some incorporate supremacist and homophobic subtitles.
“I’m moving, yet meanwhile, I need to feel safe and I need these awful animals to leave my vehicle, patio, home, and business alone!” one gathering part composed as of late.
Next Year’s Cases
That kind of dehumanization of the general population most in danger for hepatitis A will make it troublesome for general wellbeing suppliers to battle the sickness. Be that as it may, there are a couple of brilliant spots, said Morris of the CDC.
She is cheered by the sharing of data among distressed states, the brought issues to light about the issue among wellbeing divisions across the nation, and the new proposals from the CDC’s immunization warning board to make hepatitis An inoculation routine for the destitute — a general wellbeing first.
However, Morris said she doesn’t know what one year from now’s case tally could resemble.
“I am cheerful we may not see the bigger episodes that we’re seeing right now, yet it is extremely hard to anticipate,” she said.
Other general wellbeing specialists are increasingly skeptical.
“There is a valid justification to presume that this will additionally spread to different states,” Gupta cautioned. “This isn’t yet finished.”
For Howard in Kentucky, only one inquiry remains: “This is an ailment of creating nations. One needs to ask: Why are we seeing it in the U.S.?”






